There is a question that comes up in almost every initial consultation I do. Not always out loud – sometimes it arrives as a quiet aside at the end of a long explanation about bloating, or fatigue, or food reactions.
“Is what I’m experiencing… normal?”
It is a reasonable question. And the honest answer is: most people genuinely do not know what normal bowel function looks like. Not because they are not paying attention – but because nobody has ever told them.
This guide covers what the evidence suggests, how to use the Bristol Stool Chart as a practical reference point, and what to do if your pattern does not sit in the target range.
Contents
- Why most people do not know what normal looks like
- The Bristol Stool Chart – a plain-English guide
- What healthy stool actually looks like
- How often should you be going?
- Signs your bowel habit might need attention
- What affects transit time?
- When to speak to your GP
- Working with a nutritional therapist
- Key takeaways
- Frequently asked questions
1. Why most people do not know what normal looks like
The reference point problem
Most health education around digestion focuses on the extremes – severe diarrhoea or obvious constipation. The middle ground, where most functional gut issues actually live, is rarely discussed.
Without a reference point, people default to comparing themselves to what they assume other people experience. The result is that a significant number of people have been living with suboptimal gut function for years – sometimes decades – without recognising it as something worth addressing.
This is not a niche clinical observation. In practice, it is one of the most consistent patterns I see: people who have been told everything is fine, and have believed it, because they had nothing to compare their experience against.
Why GP appointments often do not cover this
A standard GP appointment is designed to rule out disease. Tests are ordered to identify or exclude serious pathology. What they are not designed to do is assess how well your gut is functioning day to day.
Transit time, stool consistency, completeness of evacuation, and post-meal discomfort patterns are not captured by routine blood work or basic investigations. This is not a criticism of primary care – it is simply a difference in what the two settings are designed to do.
If your tests come back clear but your symptoms persist, that is not the end of the conversation. It is often the beginning of a more useful one.
2. The Bristol Stool Chart – a plain-English guide
The Bristol Stool Chart was developed at the University of Bristol in the 1990s. It classifies stool into seven types based on form and consistency, and remains one of the most widely used clinical tools for assessing gut transit time.
The chart is used in gastroenterology, primary care, and functional medicine settings because it provides a standardised, validated way to communicate about something that is otherwise difficult to describe. It is simple, takes about 30 seconds to understand, and gives an immediate frame of reference.
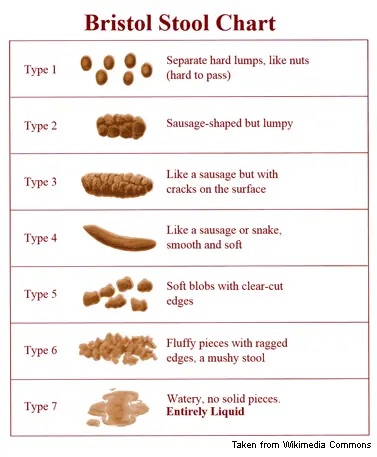
| Type | Appearance | What it suggests |
|---|---|---|
| Type 1 | Separate hard lumps – like small pellets | Slow transit / constipation |
| Type 2 | Sausage-shaped but lumpy | Slow transit / constipation |
| Type 3 | Sausage-shaped with surface cracks | Normal – target range |
| Type 4 | Smooth, soft sausage – easy to pass | Normal – target range (ideal) |
| Type 5 | Soft blobs with clear-cut edges | Borderline loose / fast transit |
| Type 6 | Fluffy pieces with ragged edges | Loose stool / fast transit |
| Type 7 | Entirely liquid with no solid pieces | Diarrhoea |
The key principle is that stool type reflects transit time. Types 1 and 2 indicate that stool has spent longer than optimal in the colon, leading to increased water absorption and harder, more difficult-to-pass stool. Types 5, 6 and 7 suggest transit is faster than optimal, with less water absorption and looser consistency. Types 3 and 4 represent the middle ground – well-formed, easy to pass, and indicative of a transit time broadly within the healthy range.
3. What healthy stool actually looks like
Healthy stool is not just about type. There are four dimensions worth considering together.
Form
Types 3 and 4 on the Bristol Stool Chart are the target. Type 4 – smooth, soft, easy to pass in one piece – is generally considered the most straightforward indicator of healthy transit.
Frequency
The clinical normal range is broader than most people realise: anywhere from three times per day to three times per week. What matters is that your frequency is consistent and that stool form is in the target range when you do go.
Ease of passing
Healthy bowel movements should require minimal effort. Straining, prolonged time on the toilet, or a sense of incomplete evacuation are all worth paying attention to – even if frequency appears normal.
Completeness
A feeling of full evacuation after a bowel movement is a useful indicator of healthy function. A persistent sense of incomplete emptying – sometimes called tenesmus – can suggest slower transit, stool consistency issues, or pelvic floor involvement, and is worth discussing with a healthcare professional.
4. How often should you be going?
The clinical definition of constipation
According to the Rome IV criteria – the internationally accepted diagnostic framework for functional bowel disorders – constipation is defined as fewer than three complete bowel movements per week, often accompanied by straining, hard stool, a sensation of incomplete evacuation, or a need to use manual manoeuvres to facilitate defecation. [2]
This is meaningfully different from the commonly held assumption that anything less than daily is problematic. Daily bowel movements are considered the gold standard, but they are not a requirement for healthy gut function.
Why daily does not automatically mean optimal
Daily type 1 or type 2 stool is a greater functional concern than type 4 stool every other day. The form tells you far more about what is happening in the colon than frequency alone.
If you are going every day but consistently passing hard, pellet-like stool with straining, your gut is not functioning optimally – regardless of the tick in the frequency box.
5. Signs your bowel habit might need attention
The following patterns are worth taking seriously, even if they have been present for a long time and feel “normal” to you.
Persistent type 1 or 2 stool
Hard, lumpy stool that is difficult to pass is the most direct indicator of slow transit. It suggests stool is spending longer than optimal in the colon, and the causes are worth investigating rather than managing indefinitely with laxatives.
Feeling of incomplete emptying
If you regularly feel as though you have not fully emptied after a bowel movement, this is worth discussing with your GP or a gut health practitioner. It can have several different drivers, and understanding which is relevant to you matters.
Bloating and abdominal heaviness
Chronic bloating – particularly towards the end of the day, or building through the week – is often associated with slower transit and stool accumulation in the colon. It is not a stand-alone diagnosis, but it is a useful signal.
Changes lasting more than four weeks
A change in bowel habit that persists for more than three to four weeks without an obvious cause warrants proper assessment, particularly in adults over 50 or in anyone with associated symptoms such as rectal bleeding, unexplained weight loss, or abdominal pain.
6. What affects transit time?
Constipation and slower transit are almost never the result of a single cause. In practice, it is usually a combination of factors that have accumulated over time.
Fibre quality and quantity
Dietary fibre is consistently associated with healthy bowel function, but type matters as much as quantity. Soluble fibre – found in oats, flaxseed, psyllium husk, and cooked vegetables – absorbs water and helps form soft, bulky stool. Insoluble fibre – found in wheat bran, raw vegetables, and wholegrains – adds bulk and can speed transit. [5]
Most people need both types, but the balance matters. Adding large amounts of insoluble fibre without adequate hydration can worsen constipation in some individuals.
Hydration
Adequate fluid intake is necessary for the colon to maintain appropriate stool consistency. Chronically low fluid intake contributes to harder stool and slower transit, particularly in warmer months or in people with high physical activity levels.
Physical movement
Physical activity has a direct effect on gut motility. The relationship is well-documented: people with sedentary lifestyles have higher rates of constipation, and even moderate daily walking can improve transit time. [3]
Stress and the gut-brain axis
The gut and the brain are in constant two-way communication via the gut-brain axis – a network involving the enteric nervous system, the vagus nerve, and the hypothalamic-pituitary-adrenal (HPA) axis. Psychological stress reliably affects gut motility, and in many people with IBS or functional constipation, stress is a primary driver of symptom fluctuation. [4]
Medication and supplements
A number of commonly prescribed medications – including opioids, iron supplements, certain antidepressants, and some antacids – can significantly slow gut transit. If you have started a new medication and noticed a change in bowel habit, this is worth discussing with your prescribing clinician.
7. When to speak to your GP
Speak to your GP promptly if you notice any of the following:
- A change in bowel habit that has persisted for more than three to four weeks without an obvious cause
- Blood in or on your stool
- Unexplained weight loss alongside a change in bowel habit
- Significant abdominal pain that is new or worsening
- A persistent feeling of incomplete emptying, particularly if this is a change from your usual pattern
- Any combination of the above
These symptoms do not automatically indicate something serious – but they do warrant proper assessment. Do not delay seeking a GP review if any of these apply to you.
8. Working with a nutritional therapist – what the process looks like
Assessment approach
When a client comes to me with constipation or concerns about their bowel habits, the process is assessment first. That means looking at transit time, stool type, frequency patterns, and symptom history alongside a detailed review of diet, hydration, stress levels, sleep, medication history, and physical activity.
The goal at this stage is not to recommend supplements – it is to understand the picture clearly enough to make decisions that are genuinely relevant to that individual.
What a structured plan looks like
Once the assessment is complete, a plan is built around the specific drivers identified. This might include dietary changes, targeted supplementation, stress management strategies, or referral for further investigation where appropriate.
What it does not look like is generic advice. Telling someone to eat more fibre and drink more water without understanding why their gut is sluggish in the first place is rarely effective long-term.
| Want to understand what is driving your symptoms?A free discovery call is a good starting point. No pressure, no obligation – just a structured conversation about where you are and whether working together makes sense. 👉 Book here |
9. Key takeaways
- The Bristol Stool Chart classifies stool into seven types. Types 3 and 4 are the target range.
- Normal bowel frequency ranges from three times per day to three times per week. Daily is not a requirement.
- Form, ease, and completeness are as important as frequency when assessing gut function.
- Types 1 and 2 suggest slow transit. Types 5, 6 and 7 suggest fast transit.
- Normal test results do not rule out functional gut issues – they rule out disease.
- Transit time is influenced by fibre quality, hydration, movement, stress, and medication.
- A change in bowel habit lasting more than four weeks warrants a GP review.
10. Frequently asked questions
What does a healthy poo actually look like?
A healthy bowel movement is typically type 3 or 4 on the Bristol Stool Chart – smooth, formed, easy to pass, and complete. It should not require significant straining, and you should feel fully empty afterwards.
Is it normal to only go to the toilet three times a week?
Yes, within a clinical context. The normal range extends from three times per day to three times per week. What matters is that when you do go, the stool is well-formed and easy to pass. If you are passing type 1 or 2 stool infrequently with straining, that is worth addressing.
Can stress cause constipation?
Yes. Stress activates the HPA axis and the sympathetic nervous system, both of which can slow gut motility. For many people with functional constipation or IBS-C, stress is a primary or contributing driver – and addressing it directly is an important part of a root-cause approach.
What is the difference between slow transit constipation and IBS-C?
Slow transit constipation refers specifically to reduced colonic motility – stool moves through the colon more slowly than normal. IBS-C (IBS with predominant constipation) is a functional bowel disorder diagnosed by symptom criteria (Rome IV) and can involve slow transit, but also includes features such as abdominal pain related to defecation. The distinction matters clinically, as the management approach can differ.
When should I be worried about a change in my bowel habit?
Any change that persists for more than three to four weeks without a clear cause – particularly in adults over 50 – warrants a GP review. This is especially important if accompanied by rectal bleeding, unexplained weight loss, or significant abdominal pain. These symptoms do not automatically mean something serious, but they should always be properly assessed.
References and further reading
[1] Heaton KW, et al. (1992). Defecation frequency and timing, and stool form in the general population. Gut, 33(6), 818-824.
[2] Mearin F, et al. (2016). Bowel Disorders. Gastroenterology. Rome IV Criteria.
[3] Johannesson E, et al. (2011). Physical activity improves symptoms in irritable bowel syndrome. American Journal of Gastroenterology, 106(5), 915-922.
[4] Carabotti M, et al. (2015). The gut-brain axis: interactions between enteric and central nervous systems in functional and inflammatory bowel conditions. Annals of Gastroenterology, 28(2), 203-209.
[5] Eswaran S, et al. (2013). Fiber and functional gastrointestinal disorders. American Journal of Gastroenterology, 108(5), 718-727.
| Educational disclaimerThis article is for educational purposes only and does not constitute medical advice, diagnosis, or treatment. The information provided is intended to support general health awareness and is not a substitute for professional medical guidance. If you have concerns about your digestive health or notice any change in your bowel habit, please consult a qualified healthcare professional. |


Leave a Reply